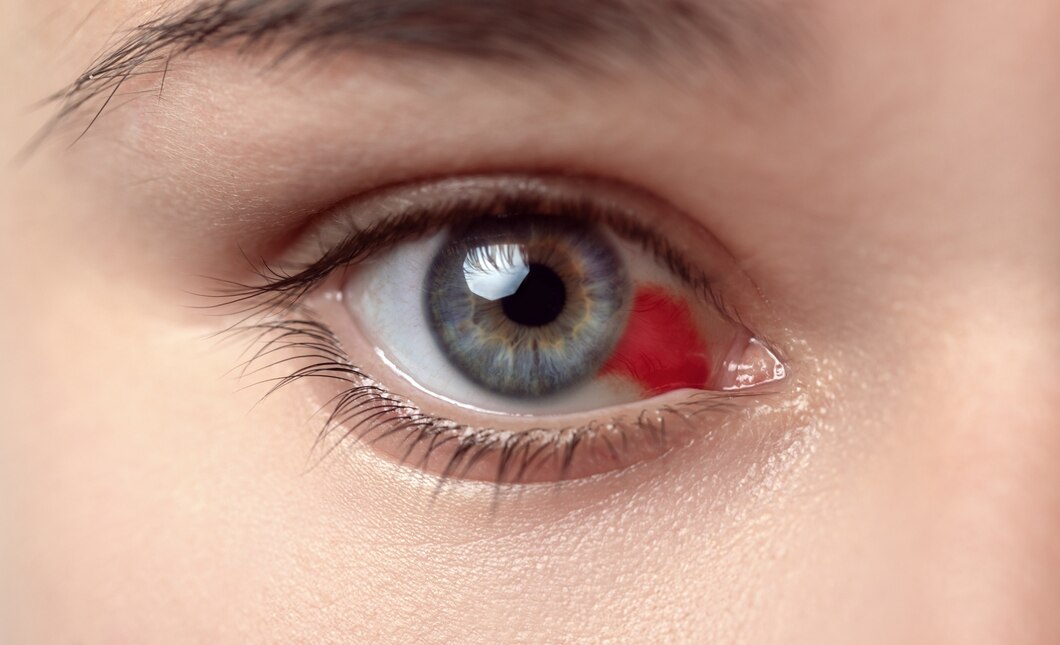
Today, I’d like to go through some basics around what to do when a child comes to the clinic with a red eye. This is a common occurrence and I like to remind our residents that the history leading up to the redness, along with the location of the redness is important in helping you to determine the differential diagnosis and cause of the red eye.
 ,
,
Source: By Eddie314 at the English-language Wikipedia, CC BY-SA 3.0
Physical Exam Tip
A child comes in with a red eye. Does the location of the redness matter?
First, “ciliary flush” refers to redness due to dilated deep conjunctival and episcleral vessels adjacent and circumferential to the corneal limbus.
DIFFERENTIAL DIAGNOSIS
For a ciliary flush includes corneal inflammation such as keratitis, iridocyclitis, uveitis, or acute glaucoma. Therefore, children presenting with a ciliary flush on exam should be seen by an ophthalmologist urgently.
FEATURES OF A DANGEROUS RED EYE
- Severe ocular pain
- Photophobia
- Persistent blurred vision or decreased visual acuity
- Proptosis
- Reduced ocular movements
- Ciliary flush
- Irregular corneal light reflection
- Abnormal red reflex
- Corneal epithelial defect or opacity
- Pupil unreactive to direct light
- Worsening signs after 3 days of pharmacologic treatment
- Compromised host: neonate, immunosuppressed patient, or soft contact lens wearer
*Taken from Jonathan D. Trobe, MD. The Physician’s Guide to Eye Care.
STEROID USE IN EYES
Do not use topical corticosteroids or corticosteroid-antibiotic combinations in treating a red eye without first consulting with an eye specialist. These agents may mask serious conditions and create others such as glaucoma, cataract, infection, and corneal perforation.
Hope this helps!
Best Regards,
Dr. Eyal Ben-Isaac, Children’s Hospital Los Angeles